The Neuropsychiatric Inventory Questionnaire (NPI-Q)
The NPI-Q helps caregivers report behavioural changes in dementia. It measures symptom severity and caregiver distress, allowing clinicians to track progress and adjust care plans.


Neuropsychiatric Inventory Questionnaire (NPI-Q)
The Neuropsychiatric Inventory Questionnaire (NPI-Q) is a brief assessment used to evaluate neuropsychiatric symptoms in dementia. It measures both symptom severity and caregiver distress, helping clinicians monitor changes. It's an essential tool for managing patient care and understanding behavioural impacts.
Category
Disease
Source
What is Neuropsychiatric Inventory Questionnaire (NPI-Q)

The Neuropsychiatric Inventory Questionnaire (NPI-Q) is a trusted instrument for assessing dementia symptoms. It tracks behavioural changes and carer stress levels. Adapted from the longer NPI, this brief version relies on informant reports. It covers twelve specific domains of neuropsychiatric functioning often affected by cognitive decline. The form looks at issues like agitation, depression, and anxiety. If a symptom is present, the caregiver rates its severity on a three-point scale. They also rate their own distress on a five-point scale, providing a clear picture of the overall burden. Clinicians use the NPI-Q in routine practice as it is fast and easy to score. It works well for monitoring treatment effects over time. By highlighting specific challenges, it helps healthcare teams create better support plans for families managing the daily reality of dementia.

The NPI-Q can be scored using two main approaches: Symptom Severity and Caregiver Distress. 1. Symptom Severity: You rate the intensity of symptoms across 12 domains like anxiety or apathy. Scores range from 1 for mild to 3 for severe. Adding these gives a total severity score up to 36, showing the overall clinical burden. 2. Caregiver Distress: This measures the impact on the carer. You rate emotional stress from 0 to 5 for each symptom present. Summing these creates a total distress score out of 60, which helps doctors identify carer burnout risks in the real world.

Advantages
Quick completion with minimal burden.
Develops personalised strategies based on assessment data.
Tracks patient condition changes systematically.
Provides consistent measurements for clinical research.
Related Instruments
Screens for neuropathic pain components.
Predicts long-term disability risk in musculoskeletal pain.
Assesses symptoms and function in lumbar spinal stenosis.
Collect NPI-Q data with WeGuide, the all in one patient engagement platform
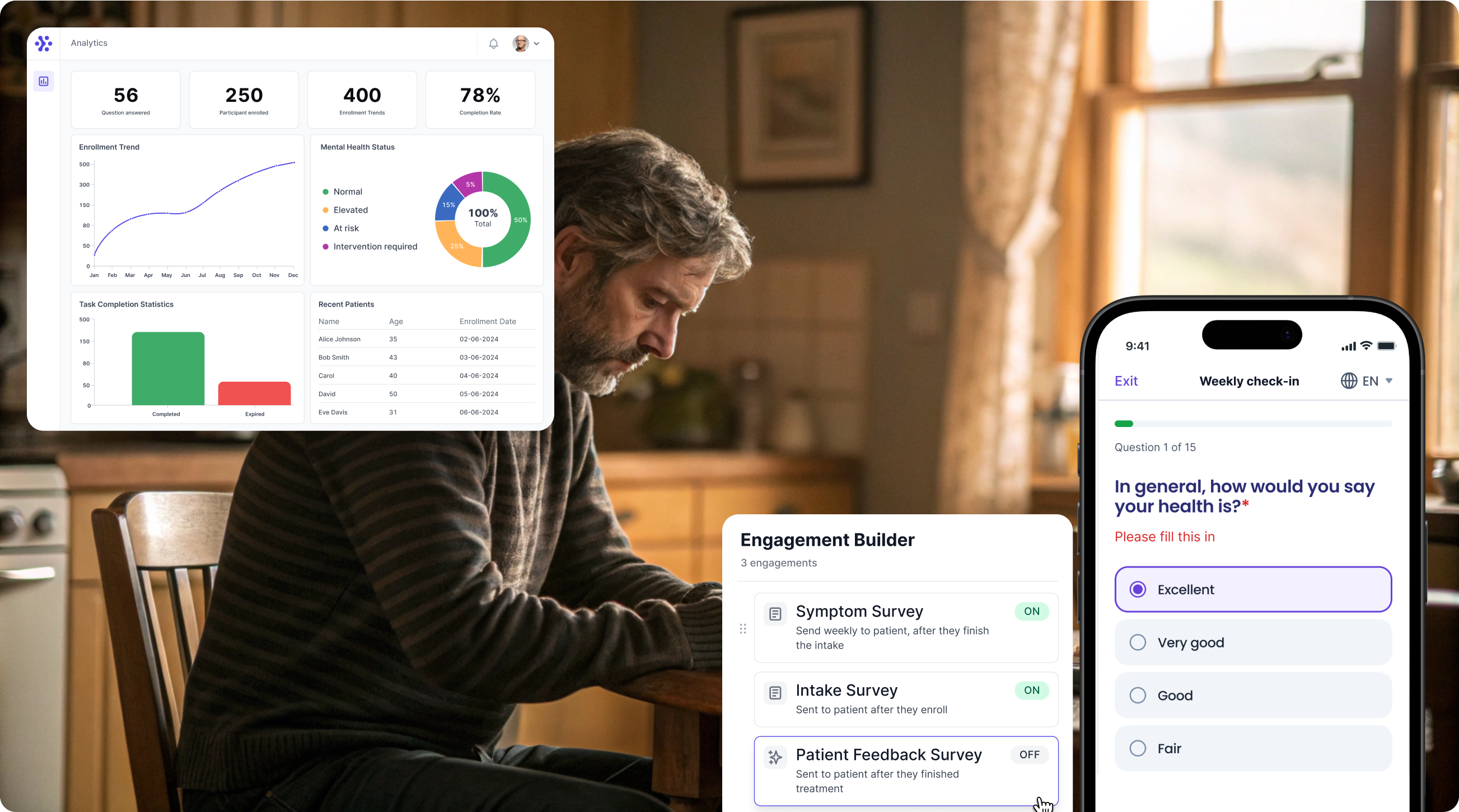

Support Your patient in no time - all under your own brand
Our platform combines the knowledge of 100+ digital health solutions built, letting you easily build your patient engagement app for research or clinical use. Collect PROMs, support patients on waiting lists, or gather vital signs data. This is how:
Learn MoreProgram Builder
.png)
Whitelabelling
.svg)
.svg)
Turn on components, dependent on your usecase
.svg)
Support The Full Journey
.png)
.png)
%20(1).png)
.png)
It’s your turn
Every WeGuide project, saves researchers and clinicians - 9 months and $450,000 - creating impactful digital health solutions.




